In the current state of the COVID-19 (Coronavirus) crisis, we MUST look for ways to give our patients the best treatment while keeping ourselves and other patients safe.
The problem is that the standard way we were practicing simply won’t suffice since the COVID-19 (Coronavirus) is so virulent and contagious. Chest Xrays and CT scans may have been ordered more liberally prior to COVID-19, but now we must really consider the risks and practicality of using these modalities in our everyday care. Furthermore, these resources are limited in most hospitals with only a hand full of technicians being able to perform these studies.
Given these limitations, Point-of-care Lung Ultrasound is becoming a very useful tool in our fight against COVID-19 (Coronavirus).
However, for some healthcare providers, it may seem difficult or intimidating to use Lung Ultrasound for COVID-19 (Coronavirus) since they feel like they don’t have enough time to perform the scan or don’t know where to start learning.
Don’t worry, I’m here to tell you that Lung Ultrasound can be performed by any healthcare provider seeing patients and can be learned in a relatively short amount of time. There is already growing evidence of how this disease process is manifesting itself with regard to radiographic findings. I was able to scan some COVID-19 patients and will show you the ultrasound findings towards the end of the post. Once you gain some proficiency you will be able to perform and interpret the Lung Ultrasound in just a few minutes or less as well!
Now some may say, “this is just like any other viral pneumonia.” It’s NOT! COVID-19 must be treated and dealt with differently. Yes, some of the lung findings are similar to other forms of viral pneumonia. However, the virulence, risk of contamination, and asymptomatic spread of COVID-19 affect how, when, and even IF we should be using Lung Ultrasound. I would actually argue for a more conservative approach to using ultrasound given how contagious and virulent COVID-19 is. Therefore, understanding not just how but when to use lung ultrasound is essential.
In this post, I want to help you get started by going over the Indications, Preparation, Technique, and Pathologic findings for Lung Ultrasound in COVID-19 (Coronavirus) patients. Okay, let’s get started!
- 1) INDICATIONS for Lung Ultrasound in COVID-19
- 2) PREPARATION for Lung Ultrasound in COVID-19
- Personal Protective Equipment (PPE) for COVID-19
- Disinfection of Ultrasound Machines
- Patient Positioning
- 3) TECHNIQUE for Lung Ultrasound in COVID-19
- 4) Lung Ultrasound PATHOLOGY in COVID-19
- Table of Pathologic Lung Ultrasound Findings in COVID-19:
- Lung Ultrasound Pathology Examples on Actual COVID-19 Patient
- 5) Rule out Alternative Diagnoses
- Summary
1) INDICATIONS for Lung Ultrasound in COVID-19
“Does it change your management?”
As an ultrasound director, I love doing educational scans to help learners get better at scanning. However, as in all test we order or think about ordering, the first questions in your mind should be “Does it change my management?” and what are the risks versus benefits of doing a test. If a patient is hemodynamically stable and is going to be discharged regardless then DON’T do unnecessary testing. In the setting of COVID-19 (Coronavirus), the risks are extremely high with regards to infecting self, staff, and other patients.
So if you are going to perform the lung ultrasound, make sure it will have potential BENEFITS such as changing treatment management or disposition.
I want to emphasize that lung ultrasound is not the determining factor for admission. It is still the patient’s clinical status (hypoxemic, tachypneic, hypotensive, etc). The main reason point-of-care ultrasound helps you here is that you can see if a patient has significant lung findings OR other possible diagnoses that can help change your management or disposition. See below for a proposed algorithm we made at POCUS 101. Feel free to download the PDF and share it with others.
Point of Care Ultrasound and COVID-19 Algorithm
2) PREPARATION for Lung Ultrasound in COVID-19
Personal Protective Equipment (PPE) for COVID-19
Prior to starting the ultrasound exam, the most important thing is to make sure you protect yourself and others. Here is a quick video on how on proper donning and doffing of PPE:
Disinfection of Ultrasound Machines
Here is a link to the official list of all the approved disinfectant wipes against COVID-19 (Coronavirus) by the United States Environmental Protection Agency.
The Canadian Point of Care Ultrasound Society came out with fantastic downloadable PDFs on protocols for disinfecting ultrasound machines (both cart-based and hand-held). Check them out below and click the image to download the PDFs! *Also consider having a dedicated ultrasound machine just for COVID-19 patients as to not transmit the disease to staff or other patients.
Patient Positioning
Depending on the severity of the COVID-19 (Coronavirus), a patient may be upright, lateral decubitus, supine, or prone. Having the patient upright or lateral decubitus will allow you access to all the lung zones, but unfortunately, most patients who have significant disease or are intubated may not tolerate these two positions.
The most common position to scan the patient will be supine with the patient’s arm abducted, but just note that you will have more difficulty accessing the Posterior lung fields in the Supine position. To get access to the subscapular area in supine patients, it may be helpful to roll the patient over to one side using a pillow or blankets to get access.
Below are figures on patient position for lung ultrasound from Havelock, et al. Thorax 65 Suppl 2(Suppl 2), ii61 – 76.



Conversely, in the Prone position, you will have more difficulty accessing the Anterior lung fields. There is a technique called the “swimmer position” described by Uglade, et al to access the anterior thorax by abducting the arm and elevating the shoulder with a pillow.

Int Care Med (2018) 44:986
3) TECHNIQUE for Lung Ultrasound in COVID-19
Probe Selection and Ultrasound Machine Preset
The two probes I feel that are most useful are the phased array and the curvilinear probes. If possible, use the curvilinear probe since it will give you improved resolution compared to the phased array and allows you to see superficial pathology better (such as subpleural consolidations). A linear probe may also be used but it won’t allow you to look for deeper pathology such as larger consolidations, air bronchograms, or significant pleural effusions. If using a Butterfly handheld device, just set the preset and it will adjust the settings for you automatically.

Set the ultrasound machine preset to the “Lung” (or Abdomen if no lung option) and make sure the indicator dot is on the upper left side of the screen.

Image Acquisition using the 12-point Lung Exam
I would recommend performing a 12-point lung exam. Normally a 6-point lung ultrasound exam described by Lichtenstein or 8-point lung exam described by Volpicelli would suffice for most lung pathology but the disease distribution seen on CT scans from COVID-19 (Coronavirus) patients shows that the lesions are patchy and may involve any part of the lung (see below for COVID-19 lung distribution on CT).

AJR 2020; 214:1–5
So you can see by just performing the 6-Point lung ultrasound exam below, you may miss lung pathology in COVID-19 (Coronavirus)

Adapted from: Lichtenstein Annals of Intensive Care 2014, 4:1
A 12-Point lung ultrasound exam will increase your sensitivity in detecting these patchy lesions. The 12-Point exam has been described in helping Italian and Chinese physicians diagnose COVID-19 (Buensenso 2020 and Peng 2020).

Adapted from: Havelock, et al. Thorax 65 Suppl 2(Suppl 2), ii61 – 76.
There is also a recent article by Soldati 2020 that suggests doing a 14-point lung ultrasound exam that includes that includes two additional points in the back, but these two additional points may be difficult to access given the scapula.

Adapted from: Soldati 2020
Depending on the patient’s condition and possible positions, some areas may not be accessible to lung ultrasound. Just try to get as many points as you can to increase your sensitivity. Now that you understand why we do a 12-point lung ultrasound exam for COVID-19(Coronavirus), watch this quick video on how to perform the lung exam:
4) Lung Ultrasound PATHOLOGY in COVID-19
Below is a summary table of the pathologic findings you may see on lung ultrasound for COVID-19. Remember that these findings can be found anywhere on the lung since COVID-19 has a multifocal distribution. You may have areas of normal lung and other areas with pathology. In mild cases of COVID-19, there may be no pathologic findings at all, but as the disease progresses you should start seeing more of these findings with the involvement of more parts of the lung.
Table of Pathologic Lung Ultrasound Findings in COVID-19:
| Lung Ultrasound Findings in COVID-19 (* Table adapted from Peng 2020) |
| Normal Lung |
| Discrete/Minimal B-lines |
| Confluent B-lines |
| Irregular and Thickened Pleural Line |
| Subpleural Consolidation |
| Small/Tiny Pleural Effusions (moderate or large pleural effusions are rare) |
Lung Ultrasound Pathology Examples on Actual COVID-19 Patient
Below are lung ultrasound pathology of an actual COVID-19 positive patient that I encountered and was able to ultrasound and upload images for you:

*Normal Patient as reference





As the COVID-19 disease progresses in patients, it can eventually lead to ARDS where there will be more prominent B-lines, consolidations, and increased overall lung involvement.
Now that you know how to identify lung ultrasound pathology for COVID-19, check out the post on how Dr. Yale Tung from Spain performed self-ultrasounds on himself after being diagnosed with COVID-19 (Coronavirus) and the daily ultrasound findings he documented on Twitter over his 3-week illness.
5) Rule out Alternative Diagnoses
As you are performing the lung ultrasound for COVID-19 findings make sure to look for other lung pathology such as Pneumothorax, Bacterial Lobar Pneumonia, COPD. Lastly, I would recommend adding a focused cardiac ultrasound to evaluate for CHF, Hypovolemia, Massive Pulmonary Embolism, Regional Wall Motion Abnormality, and Pericardial Effusion with Tamponade.
Enjoyed this Guide on Lung Ultrasound? Check out these other two posts I made for you on GUIDE to CARDIAC and MULTIORGAN ULTRASOUND in COVID-19.
A systematic review (Hosseiny 2020) reports that severe cases of COVID-19 can cause pericardial effusions/tamponade, a study from JAMA 2020 showed increased myocardial injury in COVID-19 patients, and case reports report fulminant myocarditis (Hu 2020). There is also evidence (Li 2020) that COVID-19 patients are hypercoagulable, meaning we should also be thinking about Pulmonary Embolisms in these patients.
Going over the detailed findings of each of these alternative disease processes is beyond the scope of this single post but below are some images of lung and cardiac pathology that may be of use to you:


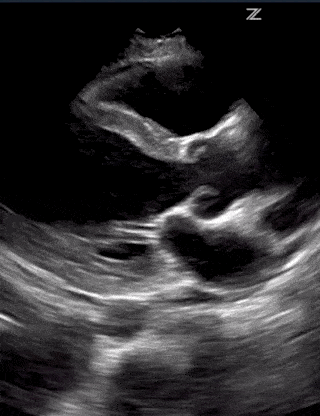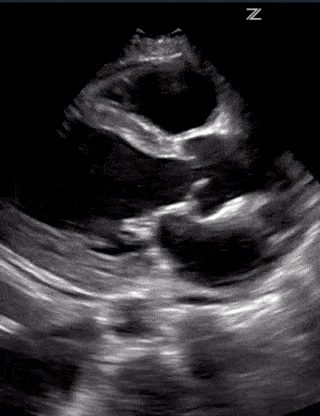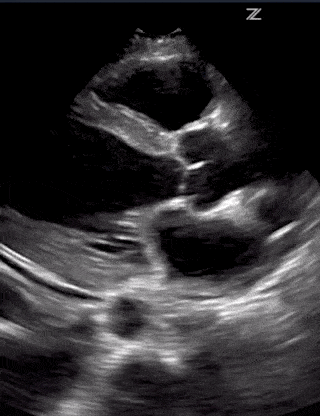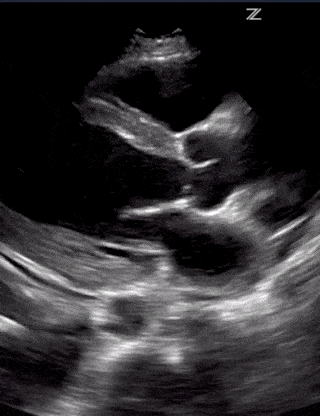


(RV Diastolic Collapse)

(RA Systolic Collapse)
Summary
I hope you found this post useful in your fight against COVID-19 (Coronavirus). It just takes a few minutes to perform the lung ultrasound exam and the COVID-19 findings are not difficult to interpret. However, remember to only perform the lung ultrasound on patients only if you think it will significantly change management or disposition.
Here is another look at the ultrasound in COVID-19 algorithm for reference:
Good luck and please stay safe. Please let me know if you have any comments or suggestions below!















Fantastic post and helpful PDF! I love seeing the global collaboration this pandemic has inspired… a silver lining in an otherwise rotten situation. Thank you for taking the time to put this together!
Thank you so much Sarah for the kind words. I’m hoping this can help as many providers as possible. I checked out your site as well. Great things you are doing on there. Stay safe!
great post.thank you so much
Thanks Roberto! I’m glad you found it helpful. stay safe!
Muy buena y didáctica!!! Felicitaciones
¡Muchas gracias! Me alegra que lo hayas encontrado útil. Buena suerte y cuídate.
awesome post, very practical and easy to use
Thanks Paresh! Thank you for the kind words 🙂
Very helpful especially for those of us in resource limited settings
Thanks Henry! Totally agree.