There has been a continual growth of evidence supporting the use of Point of Care Ultrasound (POCUS) for COVID-19 and many providers are starting to implement POCUS into their daily practice. What started out as just lung ultrasound findings for COVID-19 has developed into further “Multiorgan” findings involving the cardiovascular system. Furthermore, we are seeing COVID-19 manifest itself in different organs at different time points during the disease process (ED/outpatient versus inpatient findings).
The rate of evidence being brought forth may seem overwhelming and you may not be sure about:
- What Systems Can COVID-19 Affect?
- How Do I Integrate Lung, Cardiac, and DVT Ultrasound in COVID-19 patients?
- When Should I be Looking For Certain POCUS Findings?
- What is the Difference Between the ED/Outpatient vs Inpatient Approach for POCUS in COVID-19?
This can make you question whether you are being vigilant enough on your COVID-19 patients and giving them the optimal care they need.
Like you, I was getting frustrated by all this information and wanted to find a way to synthesize the current POCUS in COVID-19 evidence/recommendations to be used in a practical way. Working as a physician in both the Emergency Department and the Intensive Care Unit, I wanted to figure out how to best utilize a “Multiorgan POCUS Approach” in the ED/Outpatient and Inpatient Environments to help you in whatever setting you may be in.
In this post, you will learn about:
- A Downloadable PDF Summarizing a Complete Multiorgan Approach in both ED/Outpatient and Inpatient settings.
- How and When to integrate Multiorgan (Lung, Cardiac, and DVT) ultrasound in your COVID-19 Patients
- Differences between ED/Outpatient versus Inpatient POCUS approach for COVID-19
- POCUS Disease Profiles for COVID-19 patients based on the severity
This post is not just about WHAT to look for in Lung and Cardiac Ultrasounds for COVID-19 (you can read my two previous detailed blog posts on that). This article is meant to tie everything together and look at WHY and WHEN we should be performing Multiorgan POCUS in both the outpatient and inpatient settings.
The risk of transmission is extremely high, thousands of people are dying, and resources are limited. Knowing WHEN and WHY you are performing POCUS in COVID-19 has never been more important. Let’s get to it!
Table of Contents
What Organs Do COVID-19 Affect and When?
Before looking at when you should be using POCUS, you will need to first understand the stages and timing of how SARS-CoV-2 affects different organ systems. See figure below from Akhmerov 2020:

As you can see, there are 3 stages to COVID-19 that appear at different time points. Not all patients will go through the 3 stages and elderly patients or patients with comorbidities are at highest risks to go into Stages 2 and 3 of the disease (though young patients with no comorbidities may still progress through to Stage 3).
This figure is extremely important because it tells us 4 things:
- SARS-CoV-2 affects different organ systems at different times
- Most patients presenting to the Emergency Department and Outpatient settings will have just pulmonary manifestations (Stage 1 and 2) and fewer will have Stage 3
- Admitted patients have a high risk of developing ARDS, Shock, and Cardiac Failure (Stage 3). Some studies cite 20-30% of admitted patients having cardiac complications and another study showed 20% of patients with severe COVID-19 infections may have thromboembolic disease
- Therefore, we must be aware and able to assess for Stage 3 (cardiovascular) complications in our admitted patients. (Hint: we can use POCUS for this)
After initial evaluation in the emergency department, most Stage 1 patients will be discharged, Stage 2 patients will be admitted to the Med/Surg floor or step down unit, and Stage 3 patients will likely be admitted to the ICU. See below for algorithms based on these 3 stages.
Outpatient and Inpatient POCUS in COVID-19 Algorithms
I created two algorithms for you below, reflecting how to use Point of Care Ultrasound to evaluate for COVID-19 in both the ED/Outpatient and Inpatient settings based on the timing of the 3 Stages of the SARS-CoV-2 infection. We will go through the reasoning of these algorithms in detail throughout the post. Feel free to download them now!
Download PDFs Here
Emergency Department/Outpatient Assessment and Management of COVID-19 with POCUS
The Emergency Department and Outpatient settings are truly the frontlines against COVID-19. The difficulty I personally face in the Emergency Department and you might also be, is trying to determine:
- Who actually has COVID-19?
- Does POCUS Rule In or Rule Out COVID-19?
- Should You Perform POCUS on All COVID-19 suspected/confirmed Patients?
- What should I be focusing on during the POCUS exam?
Who Actually has COVID-19?
This question was very difficult to answer when we first encountered COVID-19 patients since signs and symptoms were non-specific (respiratory, GI, constitutional, etc) and tests would take days to weeks to come back. However, many hospitals now have access to COVID-19 tests that can come back in a few hours.
BUT, the caveat is that many COVID-19 tests we can have a 30% false-negative rate. So in our own practice, we still assume symptomatic patients have COVID-19, and retest 1 to 2 more times to make sure.
Either way, I believe the best approach is to assume every symptomatic patient you encounter has the COVID-19 and take appropriate precautions. Don’t let your guard down just because a test comes back negative.
Does POCUS Rule In or Rule Out COVID-19?
I’ve been getting some emails and messages about this question. I love POCUS as much as anyone else, but the simple answer is NO. POCUS is just another diagnostic tool (like CXR or CT) that helps you increase or decrease your pre-test probability of having a disease. If a patient has all of the COVID-19 typical symptoms and all of the POCUS findings, the likelihood is very high they have COVID-19, but not 100%. We have patients coming in with typical COVID-19 symptoms and radiographic findings that end up negative for COVID-19. Remember, other viral pneumonias can still present similarly.
Conversely, patients may have no POCUS findings but may still be positive for COVID-19. Usually, these patients have mild symptoms and can be discharged.
Should You Perform POCUS on All COVID-19 suspected/confirmed Patients?
Initially, there was some debate about this in the POCUS community. However, there is much more consensus within the community and societies that POCUS should only be performed IF it will change management on your patient.
Overall, vital signs seem to be fairly sensitive in determining who should be admitted or not. So if your patient has completely normal vital signs and mild symptoms, consider discharging them without POCUS. If you are concerned, there are some expert groups that suggest using outpatient pulse ox monitors like the one below to have patients self-monitor after discharge.
What POCUS Findings Should You Be Focusing on in the ED/Outpatient Settings?
Given that most patients will be in Stage 1 or Stage 2 of the COVID-19 disease process when they present to the Emergency Department or Outpatient settings, you should really be focusing on finding Lung Ultrasound abnormalities in these patients.
If you have decided to do lung ultrasound and are comfortable with performing cardiac and lower extremity ultrasounds, you should also screen for any significant cardiovascular or thromboembolic pathology at the same time. This is with the understanding that the majority of the findings you see will be pulmonary related.
However, If you do see a sick COVID-19 patient presenting to your Emergency Department, have a much higher suspicion for cardiovascular and thromboembolic involvement (Stage 3).
Inpatient Assessment and Management of COVID-19 with POCUS
The problem in the Emergency Department was trying to determine WHO has COVID-19 and to optimize initial management, however, the problem in the INPATIENT setting is HOW do I Manage and Reassess my COVID-19 Patients. So here are some Inpatient questions that you may come across:
- How Quickly can my COVID-19 Patient Deteriorate?
- When Should I Reassess my COVID-19 Patients using POCUS?
- If My Admiited COVID-19 Patient is Getting Worse, What POCUS Findings Should I be Looking For?
How Quickly can my COVID-19 Patient Deteriorate?
Every patient will develop a different reaction and time course to their COVID-19 illness. Some patients may just get better and some may rapidly progress. My personal recommendation would be to reevaluate the patient every 2-4 hours during their initial admission to make sure there are no abrupt changes in vital signs, mentation, lab values, or respiratory/cardiac symptoms.
Any significant changes can indicate an impending rapid deterioration that may require looking for life-threatening pathology, advanced airway management or intervention.
When Should I Use POCUS to Reassess my COVID-19 Patient?
Similar to the ED/Outpatient setting, you should only perform POCUS if the findings will change your management. In the inpatient setting, if there are any significant clinical changes in your COVID-19 patients, then POCUS is likely indicated.
However, if your COVID-19 patient is improving over the next few hours/days, don’t feel the need to perform Point of Care Ultrasound routinely as it is unlikely to change your management in these patients and increases the risk of COVID-19 contamination and disease transmission.
If My Admiited COVID-19 Patient is Getting Worse, What POCUS Findings Should I be Looking For?
It seems like from the current literature that about 20% of patients who get admitted for COVID-19 can have significant cardiovascular or thromboembolic complications (Stage 3).
If you feel like your admitted patient is headed in the wrong direction, POCUS is a great resource to help you rule out life-threatening causes using a combination of cardiac, lower extremity, and lung ultrasounds. The main findings you need to focus on in a quickly deteriorating patient are:
Life-Threatening Cardiovascular Complications of COVID-19:
- Acute Cardiomyopathy: from myocarditis or stress induced (Takotsubo)
- Pericardial Effusion with Cardiac Tamponade
- STEMI with regional wall motion abnormalities (sometimes patient may have normal echo, so go with the EKG)
- Massive Pulmonary Embolism
- Thromboembolic Disease: Pulmonary Embolism and Deep Vein Thrombosis
- Hypovolemia
Life-Threatening Pulmonary Complications of COVID-19:
- Tension Pneumothorax (some COVID-19 patients maybe on high PEEP setting, predisposing them to significant barotrauma)
- Worsening or Developing ARDS: look for significant changes and increases in B-lines and consolidations.
Download Multiorgan POCUS/COVID-19 PDF Algorithms Here
COVID-19 POCUS Profiles – Cardiac, Lung, and DVT Ultrasounds
It is good to know the overall profile and progression of lung and cardiac ultrasound findings for COVID-19 as the disease gets more severe. Below are some examples, but if you want more detailed guides on lung or cardiac ultrasound for COVID-19, check out my two previous posts:
COVID-19 Cardiac and Thromboembolic Disease Progression
Use whatever protocols that work best for you to obtain your cardiac and DVT ultrasound views and make sure to get multiple views to not miss any subtle pathology. To see video tutorials on how to perform these exams, click HERE for Cardiac Ultrasound and HERE for DVT Ultrasound.
Cardiac Ultrasound Pathology
Cardiac pathology can vary between patients. But it seems like myocarditis is one of the first cardiac signs with either systolic or diastolic heart failure on ultrasound, elevated troponin, and abnormal EKG findings. This can progress to pericarditis with pericardial effusion and tamponade. Severe cases can also result in STEMI as well.
Lastly, make sure to look for Right Ventricular Function. A dilated right ventricle can be due to the significant non-compliance of the lung, massive pulmonary embolism, worsening pulmonary hypertension or significant left heart disease.
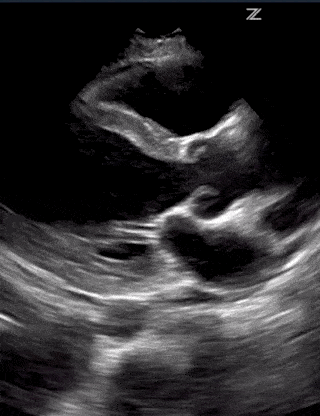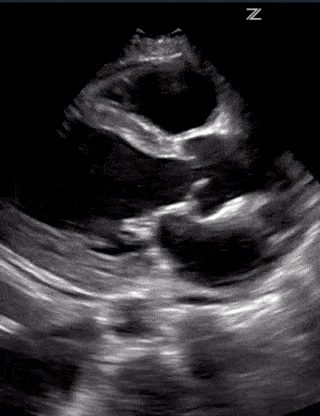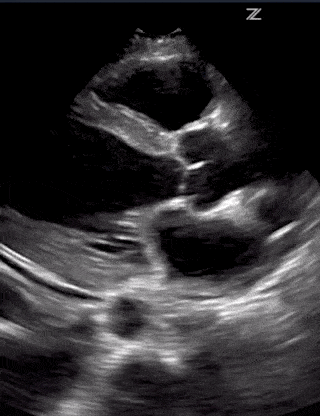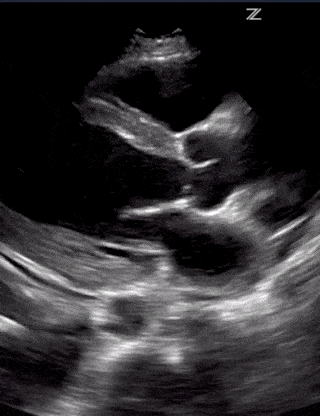

(RV Diastolic Collapse)

(RA Systolic Collapse)



DVT Ultrasound Pathology
DVT can be easily seen using ultrasound. The two main things you are looking for are direct clot visualization or a noncompressible vein (see below). If you want a more in-depth tutorial for DVT ultrasound click HERE.



COVID-19 Lung Ultrasound Disease Progression
Below is a figure from Smith, Hayward, Miller 2020, you can follow them on twitter @sonophysio. It is a great figure depicting the progression of COVID-19 lung pathology as the disease progresses. I added some video images below so you can correlate how they actually look on ultrasound. If you want lung ultrasound tutorials CLICK HERE.





I hope you found this post helpful and I would love to see any comments below on your own practice and experience!















amazing
Thanks Sadaf!
well done sadaf
Thanks, Sadaf! Hope you are doing well and staying safe :
-Vi