Primary Authors: Jessica Ahn, Vi Dinh; Co-authors: Jade Deschamps, Satchel Genobaga, Annalise Lang, Victor Lee, Reed Krause, Devin Tooma, Seth White. Oversight, Review, and Final Edits by Vi Dinh (POCUS 101 Editor).
An unrecognized or untreated Deep Vein Thrombosis (DVT) in the lower extremities is a major concern because a clot can dislodge and lead to a pulmonary embolism and hemodynamic instability.
Point of Care Compression Ultrasound is a quick and non-invasive way to assess for DVT with very high sensitivity and specificity so you can determine if anticoagulant therapy is necessary (Burnside 2008).
In this post we will show you how to use Point of Care Ultrasound (POCUS) to:
- Perform the DVT Ultrasound Exam of the Lower Extremities in a Step-by-Step Fashion.
- Evaluate for DVT using Compression, Clot Visualization, and Color Doppler Augmentation.
- Recognize DVT Ultrasound False Positives.
After learning these principles, you will be able to use Point of Care Compression Ultrasound to assess for DVTs in the lower extremities with ease! Below is a Deep Vein Thrombosis Ultrasound PDF Pocket Card you can download to help you remember the most important points.
Table of Contents
Deep Vein Thrombosis Ultrasound POCKET CARD PDF
Download DVT Ultrasound Card PDF HERE
Indications and Contraindications
Deep Vein Thrombosis Ultrasound Indications
- Unilateral lower extremity symptoms including:
- Leg pain
- Tenderness
- Swelling
- Erythema
- Positive Homans’ Sign (pain on calf compression during the physical exam)
- Any concern for DVT
Deep Vein Thrombosis Ultrasound Contraindication
- There is a theoretical risk of dislodging a clot and causing a pulmonary embolism with compression. This is a rare complication, but something you should be aware of (Lockhart, Sheldon & Robbin).
Deep Vein Thrombosis Ultrasound Preparation
Patient Preparation
- Have the patient lie supine.
- Optional: Elevate the head of the bed to 30°. This can help the blood pool in the veins of the lower extremities and aid in visualization of the vein.
- Externally rotate the patient’s leg and bend the knee into what is known as the Frog Leg position. This is the most popular position because it enlarges the vein and brings it closer to the field of vision for the plane of the ultrasound probe. In addition, the Frog Leg position allows you to scan the common femoral vein all the way to the distal popliteal vein without having to reposition the patient (Read, Holdgate & Watkins).
- Place a pillow under the patient’s knee to increase comfort.

Ultrasound Machine Preparation
- Transducer: Linear Ultrasound Probe
- Preset: Venous
- Ultrasound Machine Placement: Place the machine on the patient’s right side so you can scan with your right hand and manipulate ultrasound controls with your left hand.

DVT Ultrasound Anatomy
The venous anatomy of the lower extremity is fairly simple. Going from proximal to distal, here are the most important veins in the leg you will need to know for DVT ultrasound:
- Common Femoral Vein (CFV)
- Great Saphenous Vein
- Bifurcation of CFV into Femoral Vein (previously named Superficial Femoral Vein) and Deep Femoral Vein
- Popliteal Vein
- Trifurcation of the Popliteal Vein
- Anterior Tibial Vein
- Posterior Tibial Vein
- Peroneal Vein
The most proximal vessel is the Common Femoral Vein (CFV), which gives off an important superficial branch known as the great saphenous vein. The CFV continues on to give off a deep femoral vein, and a femoral vein.
Editor’s Note: The Femoral Vein is also previously known as the Superficial Femoral Vein. Don’t be misled by the name – the (superficial) femoral vein is actually part of the deep venous system. A study from 2011 showed that 75% of junior clinicians believed this vein was a part of the superficial venous system (Thiagarajah, Venkatanarasimha & Freeman). A clot in the (superficial) femoral vein is in fact a deep vein thrombosis and requires anticoagulant therapy to prevent a pulmonary embolus. Don’t get confused by the nomenclature!
As the femoral vein travels inferiorly and medially, it enters into the adductor canal and passes posterior to the knee to become the popliteal vein. At the level of the calf, the popliteal vein gives rise to three other deep veins: the anterior tibial vein, the posterior tibial vein, and the peroneal vein (Zitek, Baydoun & Baird).

Step-By-Step DVT Ultrasound Protocol
The 3-Point DVT Ultrasound Protocol
In this section, we will go over a step-by-step ultrasound approach to evaluate for deep vein thrombosis by visualizing the veins and using venous compression using a standard DVT Ultrasound Protocol.
It is important to note that there are several published protocols using anywhere from a 2-point ultrasound scan to a whole leg scan. We have found a 3-point compression ultrasound protocol to be most feasible while maintaining similar sensitivity and specificity when compared to a whole leg scan (Lee, Lee & Yun). We will focus on performing the 3-Point Ultrasound scan in this post, but here are the differences between the protocols that you may encounter:
2-Point Lower Extremity DVT Ultrasound: compression ultrasound including the femoral vein 1 to 2 cm above and below the saphenofemoral junction and the popliteal vein up to the calf veins confluence.
3-Point Lower Extremity DVT Ultrasound: compression ultrasound including the femoral vein 1 to 2 cm above and below the saphenofemoral junction, 1 to 2 cm above and below the bifurcation of the common femoral vein into the deep femoral vein and the (superficial) femoral vein, and lastly the popliteal vein up to the trifurcation into the anterior tibial vein, the posterior tibial vein, and the peroneal vein (Garcia 2018).
Whole Leg/Complete Lower Extremity DVT Ultrasound: involves scanning the leg using compression, color Doppler, and pulse wave Doppler from the common femoral vein all the way to the ankle while evaluating the calf veins.

Proper Vein Compression Technique
One of the biggest issues with performing DVT ultrasound is knowing how much to compress the vein. If the operator does not apply enough pressure or if the ultrasound probe is not perpendicular, these can lead to false positives for DVTs.
You should apply pressure until the pulsatile artery compresses slightly. If the adjacent vein compresses completely, there is no DVT. Refer to the figure below for an example of proper technique. If the vein does not compress completely, it is likely the patient has a clot in that region.

Editor’s Note: There is a theoretical risk of dislodging a clot and causing a pulmonary embolism with compression. This is a rare complication, but something you should be aware of.
Step 1: Scan the Common Femoral Vein
- Apply gel onto the probe and place it along the inguinal ligament midway between the pubic symphysis and the anterior superior iliac spine (ASIS).
- Orient the probe perpendicular to the skin with the indicator facing the patient’s right to obtain the transverse view.


- Locate the common femoral vein and artery.
- Notice the CFV is medial to the CFA.
- Apply firm pressure with the ultrasound probe until the artery compresses slightly. In a normal scan, the vein should compress entirely.


Step 2: Scan the Great Saphenous Vein
- Slide the probe 1-2 cm down the patient’s leg to find where the great saphenous vein branches off of the CFV.


- Keep the vessels centered in the image. As the probe moves distally, the artery will typically bifurcate first and then the vein.
- Compress the CFV at the junction with the Great Saphenous Vein.
- Editor’s Note: Depending on the size and proximity of a clot in the great saphenous vein to the CFV, there is evidence that these should be treated as DVT too.


Step 3: Scan the (Superficial) Femoral Vein
- Slide the probe 1-2 cm down the patient’s leg to find where the CFV branches into the deep femoral vein and (superficial) femoral vein.


- At this point, the deep femoral vein will dive deep in the thigh. However, the (superficial) femoral vein will travel alongside the femoral artery.
- Compress the (superficial) femoral vein just distal to the bifurcation.
- Optional: though the 3-point ultrasound protocol only requires you to compress just distal to the bifurcation, you can also periodically check for clots in the rest of the (superficial) femoral vein using compression as you gradually move the probe inferiorly and medially towards the popliteal fossa where the (superficial) femoral vein dives into the adductor canal.


Step 4: Scan the Popliteal Vein
- Move the probe into the posterior crease of the knee and scan 2 cm above and below to find the popliteal vein.
- POCUS 101 Tip: Sometimes it is difficult to locate the popliteal vein when you first start scanning. An easy way to locate it is to place the probe directly in between the two hamstring tendons behind the knee.


- Use the probe to compress the popliteal vein and check for clots.
- Editor’s Note: Notice in this view that the popliteal vein is now on top and the popliteal artery is on the bottom. Think “Pop on Top!“


Step 5: Scan the Trifurcation of the Popliteal Vein
- Continue to scan slightly more distal from the popliteal vein to find its trifurcation.


- Compress the popliteal vein periodically until you find where the popliteal vein trifurcates into the anterior tibial, peroneal, and posterior tibial veins. This junction signals the end of the examination.

Deep Vein Thrombosis Ultrasound Pathology Overview
Deep vein thrombosis can be detected in three ways using point of care ultrasound: direct clot visualization, non-compressibility of vein, and augmentation with Color Doppler.
Direct visualization of the echogenic clot with ultrasound is a definitive way to detect a DVT. Among the indirect ways for diagnosing a DVT, compression ultrasound provides the highest sensitivity and specificity. A study of 220 symptomatic patients scanned for DVT with compression ultrasound yielded a 100% sensitivity and 99% specificity (Lensing et al, 1989). In comparison, augmentation with Color Doppler does not improve the accuracy of scanning and requires squeezing the patient’s leg, which could dislodge any present clots and cause a pulmonary embolism (Lockhart, Sheldon & Robbin; Blaivas et al).
Our recommendation to diagnose DVT is to first use the direct visualization technique. If an echogenic mass is not apparent, we recommend evaluating the compressibility of the veins. The use of color Doppler and augmentation are optional modalities.
Remember to download the DVT Ultrasound Pocket Card PDF as a reference for DVT Ultrasound technique, pathology, and false positives:
Download DVT Ultrasound Pocket Card PDF HERE
Direct Clot Visualization with Ultrasound
Depending on the age of a clot, you may see an echogenic mass inside the vessel on ultrasound if your probe is directly over the mass. You may not be able to see acute thrombi because they are anechoic or hypoechoic and they tend to be near the edges of the lumen. As the thrombus ages, it becomes more echogenic and retracts from the vein walls, making it much easier to detect with ultrasound. Therefore, when scanning for clots, do not just rely on direct visualization and always be sure to perform the compression technique to not miss any acute DVTs.
Examples of Direct Clot Visualization of DVT


Non-Compressibility with Ultrasound
You can also detect a DVT by compressing the veins. If you apply pressure with the probe until the artery compresses slightly and the vein compresses completely, there is likely no DVT at that spot. However, if you apply enough pressure that the artery compresses but the vein does not compress completely this is considered a “non-compressible” vein and it is likely the patient has a clot in that region.
Examples of Non-Compressible Veins of DVT



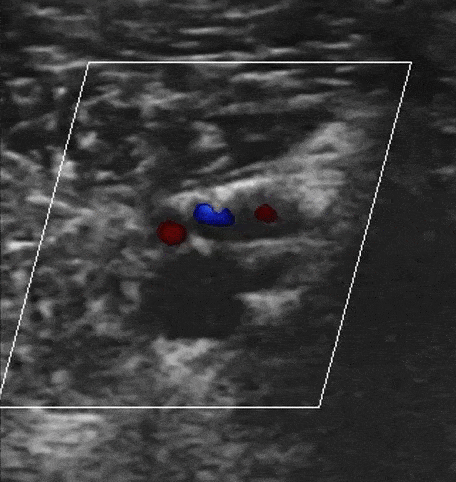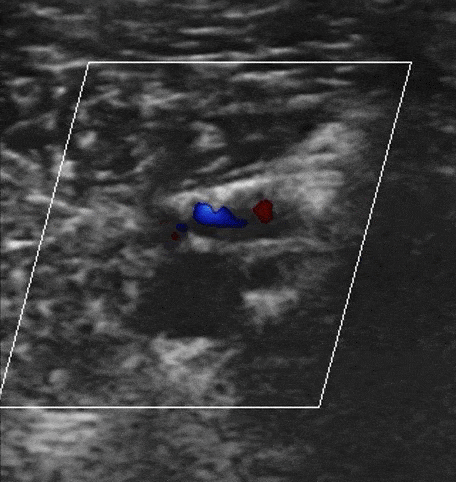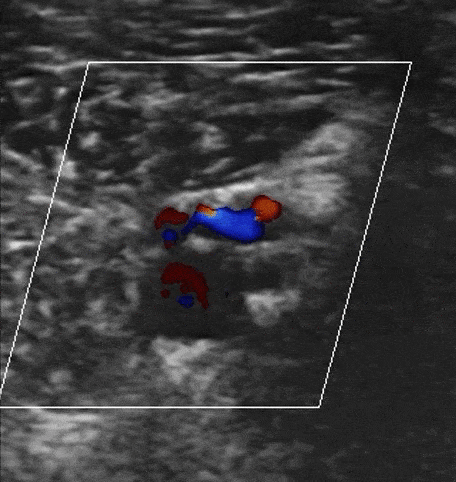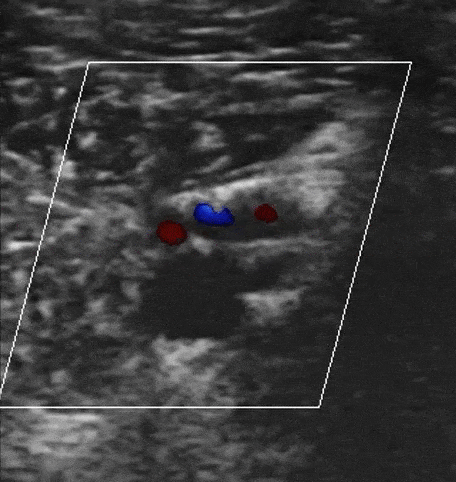
Augmentation with Color Doppler
You can augment venous flow by squeezing the leg distal to where you are scanning. If Color Doppler demonstrates a homogenous increase in venous flow, this suggests that there is no occlusive thrombus between where you are squeezing and scanning. However, if there is no increase in venous flow, there could be a DVT.
Editor’s Note: Use this method with caution as there could be a risk of dislodging any existing clots and causing a pulmonary embolism.
Obstructed Veins with Color Doppler of DVT


Video Summary for DVT Ultrasound
Below is a video we made summarizing how to obtain the views for DVT ultrasound as well as how to evaluate for DVT pathology:
Deep Vein Thrombosis Treatment
It is important to treat DVT since one out of three patients with untreated DVT experience clinically significant pulmonary embolism, and the short-term mortality rate from untreated PE can exceed 20% (Burnside et al).
It is beyond the scope of this post to explain all of the possible treatments for DVT, but here is a proposed algorithm adapted from Mazzolai 2017:

Deep Vein Thrombosis False Positives
There are a few structures that can be mistaken for a deep vein thrombosis because they look like non-compressible vessels. These include superficial thrombophlebitis, Baker’s cysts, lymph nodes, pseudoaneurysms, and groin hematomas, which we will show below.
To help avoid these false positives, be sure to always identify that the vein is next to an artery. Additionally, if you compare the vein in Short Axis and Long Axis views, it will look circular in the short axis view and cylindrical in the long axis view.


Superficial Thrombophlebitis
Superficial thrombophlebitis occurs when there is a clot in a superficial vein, like the great and small saphenous veins and the varicose veins.
A clot in a superficial vein will show the same signs on ultrasound as in a deep vein; you can see an echogenic mass with direct visualization, non-compressibility, and decreased or absent color flow. The major difference is that superficial veins do NOT accompany arteries while deep veins do (Naringrekar et al).
This pitfall is more likely in obese patients whose superficial veins are enlarged and can be mistaken as deep veins.

Baker’s Cyst
A Baker’s cyst is a fluid-filled cyst in the popliteal bursa on the back of the knee. This can result from inflammation of the knee joint or a knee injury, like a cartilage tear.
These popliteal cysts can present with similar symptoms as a deep vein thrombosis such as sharp knee pain, calf swelling, and occasionally erythema.
On ultrasound, a Baker’s cyst appears as a circular anechoic mass with sharply defined borders in both the longitudinal and transverse view (Zitek, Baydoun & Baird). On Color Doppler, there should be no flow.


Lymph Nodes
Lymph nodes are part of the adaptive immune system and can become inflamed when the body is fighting an infection.
On ultrasound, a lymph node can look similar to a clot because it is a hypoechoic oval structure with a hyperechoic center. However, if you scan the lymph node in the longitudinal view, it becomes apparent that the object is circumscribed and not tubular in structure like a vein (Zitek, Baydoun & Baird). Lastly, a lymph node will disappear quickly if you attempt to trace it up and down, unlike an artery or vein that will be continuous structure.

Pseudoaneurysms
A pseudoaneurysm occurs when there is a partial rupture of an artery wall that leads to an outpouching of the artery with the accumulation of periarterial blood. This most commonly occurs from arterial trauma from an interventional medical procedure, gunshot, or a stab wound (Montorfano et al). These sites can become infected and give off emboli.
On ultrasound, pseudoaneurysms present as anechoic or hypoechoic images, sometimes with moving echoes. With Color Doppler, you can see a “Yin-Yang Sign” from the circular motion of blood inside the pseudoaneurysm cavity. In systole, blood flows towards the pseudoaneurysm cavity (red) while in diastole the blood moves back towards the arterial lumen (blue)(Montorfano et al).

Groin Hematoma
A groin hematoma occurs when blood leaks from an artery, typically the femoral artery, and causes localized swelling. Some risk factors can include recent procedure in that area, obesity, anticoagulation, and peripheral vascular disease (Kosmidou & Karmpaliotis).
On ultrasound, a groin hematoma will be hypoechoic with some anechoic areas scattered throughout. If you scan the hematoma in the longitudinal view, it becomes obvious that the object is circumscribed and not tubular like a vein or artery.

References
- Blaivas, M., Lambert, M., Harwood, R., Wood, J., Konicki, J. (2000). Lower-extremity Doppler for Deep Venous Thrombosis—Can Emergency Physicians Be Accurate and Fast? Academic Emergency Medicine 7(2), 120-126. https://dx.doi.org/10.1111/j.1553-2712.2000.tb00512.x
- Burnside, P., Brown, M., Kline, J. (2008). Systematic review of emergency physician-performed ultrasonography for lower-extremity deep vein thrombosis. Academic emergency medicine : official journal of the Society for Academic Emergency Medicine 15(6), 493-8. https://dx.doi.org/10.1111/j.1553-2712.2008.00101.x
- Chong, V. (1996). Calf pain and swelling: Baker’s cyst mimicking deep vein thrombosis. Singapore medical journal 37(2), 175-80.
- García, J., Alonso, J., García, P., Rodríguez, F., López, M., Muñoz-Villanueva, M. (2018). Comparison of the Accuracy of Emergency Department-Performed Point-of-Care-Ultrasound (POCUS) in the Diagnosis of Lower-Extremity Deep Vein Thrombosis The Journal of Emergency Medicine 54(5), 656-664.
- Kosmidou, I., Karmpaliotis, D. (2010). Cardiac Intensive Care Section III: Coronary Artery Disease: Complications of Percutaneous Interventional Procedures https://dx.doi.org/10.1016/b978-1-4160-3773-6.10023-0
- Lee, J., Lee, S., Yun, S. (2019). Comparison of 2-point and 3-point point-of-care ultrasound techniques for deep vein thrombosis at the emergency department: A meta-analysis Medicine 98(22), e15791.
- Lockhart, M., Sheldon, H., Robbin, M. (2005). Augmentation in Lower Extremity Sonography for the Detection of Deep Venous Thrombosis American Journal of Roentgenology 184(2), 419-422.
- Mayo Clinic. https://www.mayoclinic.org/diseases-conditions/bakers-cyst/symptoms-causes/syc-20369950
- Mazzolai, L., Aboyans, V., Ageno, W., Agnelli, G., Alatri, A., Bauersachs, R., Brekelmans, M., Büller, H., Elias, A., Farge, D., Konstantinides, S., Palareti, G., Prandoni, P., Righini, M., Torbicki, A., Vlachopoulos, C., Brodmann, M. (2017). Diagnosis and management of acute deep vein thrombosis: a joint consensus document from the European Society of Cardiology working groups of aorta and peripheral vascular diseases and pulmonary circulation and right ventricular function European Heart Journal 39(47), 4208-4218.
- Montorfano, M., Pla, F., Vera, L., Cardillo, O., Nigra, S., Montorfano, L. (2017). Point-of-care ultrasound and Doppler ultrasound evaluation of vascular injuries in penetrating and blunt trauma Critical Ultrasound Journal 9(1), 5. https://dx.doi.org/10.1186/s13089-017-0060-5
- Naringrekar, H., Sun, J., Ko, C., Rodgers, S. (2019). It’s Not All Deep Vein Thrombosis: Sonography of the Painful Lower Extremity With Multimodality Correlation Journal of Ultrasound in Medicine 38(4), 1075-1089. https://dx.doi.org/10.1002/jum.14776
- Nasr, H., Scriven, J. (2015). Superficial thrombophlebitis (superficial venous thrombosis) BMJ 350(jun22 6), h2039-h2039. https://dx.doi.org/10.1136/bmj.h2039
- Ony, L., Rafaralahivoavy, T., Ahmad, A., Rakoto, A. (2013). Hematoma – Abscess of the Psoas and Hemophilia: About an Adult Case Cureus 5(2), e91. https://dx.doi.org/10.7759/cureus.91
- Prativadi, R., Dahiya, N., Kamaya, A., Bhatt, S. (2017). Chapter 5 Ultrasound Characteristics of Benign vs Malignant Cervical Lymph Nodes Seminars in Ultrasound, CT and MRI 38(5), 506-515.
- Read, H., Holdgate, A., Watkins, S. (2012). Simple external rotation of the leg increases the size and accessibility of the femoral vein Emergency Medicine Australasia 24(4), 408-413. https://dx.doi.org/10.1111/j.1742-6723.2012.01568.x
- Thiagarajah, R., Venkatanarasimha, N., Freeman, S. (2011). Use of the term “superficial femoral vein” in ultrasound Journal of Clinical Ultrasound 39(1), 32-34. https://dx.doi.org/10.1002/jcu.20747
- Zitek, J., Baydoun, J., Baird, J. (2013). Tools for the Clinician: The Essentials of Bedside (ED or ICU) Ultrasound for Deep Vein Thrombosis Current Emergency and Hospital Medicine Reports 1(2), 65-70. https://dx.doi.org/10.1007/s40138-013-0016-4
- Lensing, A., Doris, C., McGrath, F., Cogo, A., Sabine, M., Ginsberg, J., Prandoni, P., Turpie, A., Hirsh, J. (1997). A Comparison of Compression Ultrasound With Color Doppler Ultrasound for the Diagnosis of Symptomless Postoperative Deep Vein Thrombosis. Archives of Internal Medicine 157(7), 765.











[…] DVT Ultrasound Tutorial […]
Very informative! Would it be possible to link to one of the videos in a publication?
Hi Josh! Yes of course feel free to link the videos into your publication. -Vi Dinh
Thank you!!
thx so so so so much
Yes of course! Anytime!
Amazing, thank you so much,have not found better material online
Thanks so much Marek! Really appreciate the comment. It means a lot.
Anything like this for upper extremity vascular exams??? Sooo helpful for lower extremity…need upper extremity and ABI
Hi we haven’t made this yet but will keep it on the list of blog post to do in the future! Thanks for the feedback.
[…] https://www.pocus101.com/dvt-ultrasound-made-easy-step-by-step-guide/#Step-By-Step_DVT_Ultrasound_Pr… […]
Amazing tutorial! Would it be possible to use the images and the gifs for a presentation?
Hi Vincenzo,
Please email me directly at editor@Vi Dinh.com for specific images you will be using and permission. Thanks!